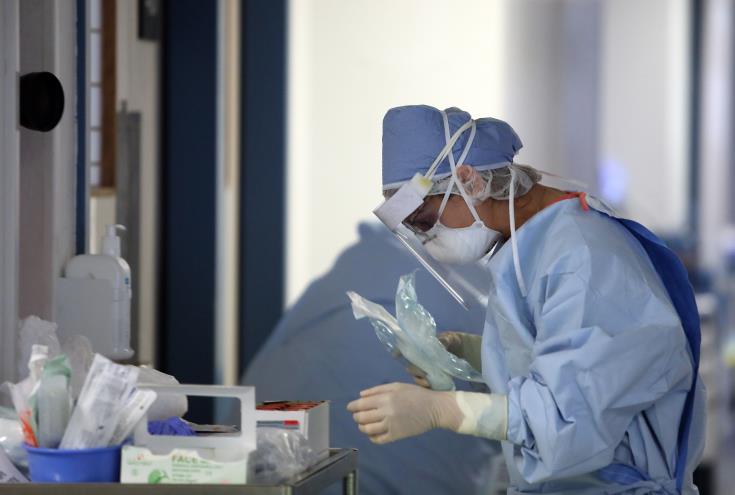
State doctors’ demands and the Health Ministry succumbing to pressure, especially in an election year, suggests that patient rights have been thrown out with the bedpan.
The public watches with awe the latest saga in the deteriorating public health sector, with the ‘new’ initiative of outpatient services provided by GPs and paediatricians over weekends, and late evenings, soon to become a non-starter.
And they are scheduled to start on 9 July.
State doctors do not want to compare or compete even with their private-sector colleagues and are scheming all sorts of excuses to prevent this from happening.
For over two years, we have been told that doctors working in public hospitals were overworked, underpaid and fleeing in droves, a myth demolished by the Auditor General in parliament this week.
He said that patient admissions in state hospitals had dropped while the number of doctors remained almost unchanged.
Interestingly, non-medical admin staff increased fivefold, indicating that work was finally being done, at least the paperwork.
This should have been tagged as a misnomer as with the introduction of online platforms by the national health service GHS; administrative work should have been simplified and speeded up.
After months of consultation, the legality of providing workspaces in the urban and regional health centres has suddenly cropped up.
This would have allowed private GPs and paediatricians to be on rotation at these centres for non-surgical and non-emergency visits.
The excuse this time is that if private physicians start using these vacant rooms, this would be the first step in privatising these centres.
How state doctors came up with this theory and how susceptible the Health Ministry has been to these arguments is anyone’s guess.
In principle, we have yet to see state hospitals become fully autonomous, sticking to a performance-based budget.
The flawed argument, in this case, has been that state hospitals provide essential services unmatched by the private sector.
These are problems that could have been resolved within days or even hours.
But no one has the political will to do so.
A representative of the patients’ association even alleged that the health sector was a state-within-a-state, run by a handful of people.
It took three decades for the GHS to take shape finally.
And when it did so, it had inexcusable teething problems, considering the millions that have been paid to consultants, experts and even system developers.
If everyone in the public health sector decided to do their work properly, efficiently, and with a general attitude of cooperation, we would never have any of these problems.